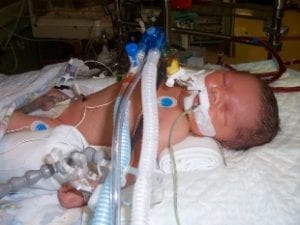
Ciaran was born on March 20th 2008 by emergency C-section after I was diagnosed with pre-eclampsia, weighing a healthy 7lb 4oz. Scans during my pregnancy had shown nothing wrong, so when he was born blue and whisked away for oxygen I assumed it was just down to his birth and he would be back soon. Hours later, doctors came and spoke to me about a condition I had never heard of – Congenital Diaphragmatic Hernia. The situation was grave, and they were giving him just a 5-10% chance of survival.
Two days after birth, after ventilation and oscillation had proved to be unsuccessful and with Ciaran’s life hanging in the balance, he was transferred from the Queen Mother’s SCBU to Yorkhill Children’s Hospital’s NICU and placed on ECMO. Now, we were told it was 50/50, and it was a waiting game to see how he would progress.
X-rays and scans had suggested that Ciaran may also have a heart condition. He had a double aortic arch and his blood vessels did not flow in a normal direction. They seemed to be in an arrangement that his doctors had never seen before, and so they did not know if this was going to need surgery. Thankfully, further tests showed that although his heart was different, it did not seem to be causing a problem. Because of this, and because he was being kept stable by ECMO, the doctors were able to try a new treatment on Ciaran. They began to fill his lungs with an oxygen-carrying fluid called PFC in an attempt to encourage them to distend. This procedure was still a part of medical research, and as far as we knew Yorkhill were the only hospital in the world to be trying it, so of course there were risks involved. But of the 14 CDH babies they had tried it on up to then, 10 had survived. So with those increased odds, we went for it.
After nine days on ECMO, and two days of the PFC treatment, we received a call to say to come to the hospital right away. Ciaran had suffered a brain haemorrhage, caused by the heparin used in the ECMO system. He needed to come off ECMO right away, which was a potential problem as they had planned to wean him off it over the space of a few days, and only when they felt his body was ready. But this was an emergency, any longer and he could bleed to death. He needed to be taken for an MRI to assess the damage done to his brain, but the doctors weren’t sure that he was strong enough to survive the journey down the stairs to the department. I wept and wept, convinced my baby boy was going to die.
He surprised us all, and seemed to do well back on a conventional ventilator. The brain scans showed that the bleed had been at the back of his brain, an unusual place for it to happen in a child – but had it happened in an adult they most probably would not have survived. The blood had gathered on his cerebellum and clotted, causing fluid to start to build up in his head, and they were tapping his head every few days to help drain some of this and take the pressure off. Other than this, he seemed to be doing well and finally, at 19 days old, he was strong enough to have his diaphragm repair.
Three hours (and three surgeons!) later, he was back on the ward with all his organs in their rightful place. The hole had been huge, and he needed a goretex patch both inside and out, as the skin on his tummy wouldn’t stretch far enough to close the wound. A week later, he had a second operation to remove the outer patch and he was left with a huge scar stretching from his left side all the way up to his right nipple.
The doctors had warned us that Ciaran was likely to do great in the first few days after surgery, but that it always happened that way and then they would expect him to get worse. The calm before the storm, sort of thing. We waited and waited for the storm, but it never came and he went from strength to strength. He came off his ventilator and onto CPAP, and we got our first cuddles when he was 4 weeks old.
His head was a different issue though, and the fluid was not going away. He needed to have further surgery to drain some of the blood clot. A specialist neurosurgeon was called in from another hospital for the case, and she wanted to have the clot assessed because she wasn’t sure it was just a blood clot, she thought he may also have cysts on his brain. The procedure would be dangerous, and difficult, but until they knew what the problem was, they couldn’t fix it. It went well though, and when the biopsy came back from the sample they found it was just blood, no cysts. Because they had drained some of the blockage they thought he might be able to manage his brain fluid better and it would not need to be tapped so much, fingers crossed.
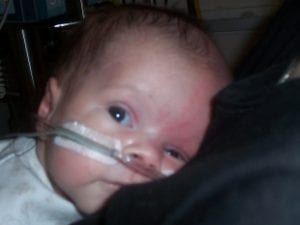
From there, Ciaran got better and better – oxygen was reducing a little more all the time while feeds were going up. Eventually he was able to take a little breastmilk from a bottle, although he was never able to breastfeed properly I felt great knowing I was able to do this one little thing to help him get stronger. At 6 weeks old he was moved out of his incubator into a cot, and out of NICU into another bed bay down the ward. Now he was no longer classified as critically ill, and it was a day we had thought we would never see. We were over the moon.
Neurologists had come to assess Ciaran and had suggested that he was showing signs of delay that may be evolving cerebral palsy, they knew his brain was damaged as a result of the haemorrhage, the clot and the hydrocephalus, but at this point they could not say how much damage was done. Taking everything into account, he said, it was highly likely that Ciaran would be very severely disabled, possibly never able to walk or communicate properly. We accepted that though, thinking that as long as he was alive, we could cope with any problems he would have. He was assigned a physiotherapist, speech and language therapist and an occupational therapist, and they visited Ciaran on the ward regularly to assess his progress and show us things we could do to help him.
At 8 weeks old, talk of home began. Ciaran was still on oxygen, but they had decided that they weren’t doing anything in the hospital that couldn’t be done at home, and so a home oxygen supply was ordered and the plans began to be set in motion for our little guy to come home. We learned to change his NG tube, did a course on baby CPR and learned how to administer all of his medications, and how to spot any signs of problems with his conditions. We were so close, and all of a sudden – a setback. Ciaran had contracted NEC, an infection of the bowel, and needed antibiotics quickly. Otherwise, they said, further surgery might be needed if his bowel was allowed to get too badly damaged. Thankfully, the antibiotics were enough to control the infection but it set him back miles with his feeding, and he now refused to feed from a bottle at all. Slowly, he came off all the drips etc that he needed after the infection, and finally on 9th June, at 11 weeks exactly, we were able to take him home on pass for one night. It was amazing having him at home, where he belonged, and the next day when we took him back to the ward, they were happy with how we had got on and how he looked and said “OK, you can take him for the weekend!”. Fantastic news, given that not 3 months earlier he had the best doctors in the country believing that he would not survive the night. After that weekend, we took him back for one night and they discharged him – we had our baby boy home for good. Or so we thought.
Three weeks after we had him home, things had been going great, until he started vomiting green bile everywhere. He would not feed, and could do nothing but throw up. I rushed him back to Yorkhill, and he was admitted again. I was devastated, more so a week later when they finally found the reason for his severe vomiting. His diaphragm had reherniated, and he would need another operation to fix it.
This time, the surgery took seven long, painful hours. His organs had fused together from the last repair, and they had to separate everything before they could even think about closing the hole. There was a lot of bleeding, but he came through and with a second goretex patch his diaphragm was repaired again. He was kept in intensive care on a ventilator for a week, and after three weeks we got him home again, just in time for his christening. We had a huge party, it was so much more than just a christening. We were welcoming home the baby boy we thought we’d never get to see grow up.
A few months later, at a routine check up with his surgeon, it was decided that his head was still growing at an alarming rate. At six months old it was the size it should be at over a year. A shunt was needed, and in October 2008 he had his seventh operation to insert a shunt in his head. This would do the job of the damaged ventricle in his brain, and drain the fluid through a tube that ran from his head to his abdominal cavity. The shunt was to be a permanent fixture in his body, he will have it for the rest of his life.
In December, at another routine check up, an x-ray showed something his consultant had never seen before – he had reherniated again. This time, it was not so severe as before and he was not showing any symptoms or any discomfort. It had to be fixed though, before it did cause a problem. A few months later he was admitted yet again for a third diaphragm repair, and a third goretex patch. It was the first time his surgeon had ever done a third repair on a CDH patient, and we are hoping beyond hope that that was rare enough that he will never need a fourth.
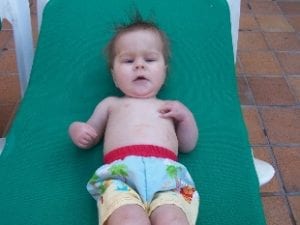
Ciaran continued to develop well beyond what the neurologist had ever expected of him. At 8 months his NG tube came out and he ate the same lumpy foods that any healthy baby his age would be eating, and he could finger feed. His speech came on beautifully, and far from not being able to communicate, he had a good vocabulary by the time he was 1. He was late to do physical things, but eventually they came. He sat up by himself for a few seconds at 10 months old. He started commando crawling at 15 months and by 16 months he was rolling over, and soon he could pull up on the furniture and over time, he learned to crawl properly, and to cruise. First one way, then the other. He was officially diagnosed with cerebral palsy at 18 months, but the neurologist who had been so pessimistic about his outcome could not believe his eyes when he saw just how far Ciaran had come. He said when he saw Ciaran’s name on his list, he expected to see a baby still on pureed foods, who could not support his head let alone sit up and move around by himself. He defied all of the textbooks.
Ciaran is now 3 years old, has been off all medication for 2 years and has, one at a time, been discharged from almost all of the specialists he once saw. He still has 6-monthly x-rays and check ups with his consultant, and still sees his physiotherapist about once every 6 weeks. He can’t yet walk or stand unsupported, and has a higher risk of chest problems than a “normal” child, but those issues aside you would never look at him and think he had been so close to not being here, or that he has been through a fraction of what he has. He is a happy, cheeky, normal 3 year old, who just needs a little extra help to get around. He needs glasses, and recently had his ninth operation to correct a squint caused by the hydrocephalus. He goes to a mainstream nursery, and is a very intelligent little boy who can count to twenty, count backwards from 12, recognise shapes, colours, numbers and letters and he has the memory of an elephant. He amazes me more and more every day, and I am prouder of his achievements than I could ever put into words.